In this post we discuss a simple and practical method of classifying periapical pathology that can be used in practice on a daily basis.
Listen to the audio version here (5 mins, 50s) : Pulpal and Periapical Diagnosis
References referred to in the episode:
Abbot P. 2004. Classification, diagnosis and clinical manifestations of apical periodontitis. Endodontic Topics 2004, 8, 36–54
Andreasen FM. Transient apical breakdown and its relation to color and sensibility changes after luxation injuries to teeth. Endod Dent Traumatol. 1986 Feb;2(1):9-19.
Eliasson S, Halvarsson C, Ljungheimer C. Periapical condensing osteitis and endodontic treatment. Oral Surg Oral Med Oral Pathol. 1984 Feb;57(2):195-9.
Johnson W. 2002. Color atlas of Endodontics. W.B. Saunders, Philidelphia
Episode Transcipt:
Welcome to the Endospot episode 3. We’re now coming to you from Brisbane, Australia.
Well, the big news for me since the last episode is that I’ve moved home from Shanghai and have set up practice in Brisbane, Australia. It’s been an interesting process setting up a practice. There are lots of buying decisions to be made and I’ll probably talk about those in some upcoming blog posts so get on to the website at www.endospot.com and remember you can sign up to have the blog posts delivered directly to your email box.
Today we’re going to quickly go through the clinical classification system that I use for periapical pathology. If you’ve listened to the last episode, you’ll remember that I like to split up my diagnosis into pulpal and periapical diagnoses. If you haven’t listened to it, do so after this podcast is finished.
As with the pulpal diagnoses, there are quite a few different systems for classifying periapical conditions, and the one I like to use is similar to that published in Johnson’s clinical atlas of endodontics. I like it because it’s simple and easy to apply clinically, and will definitely help you arrive at a treatment plan.
The first diagnosis is the obvious one, “healthy periapex”. Usually, this will accompany a healthy pulp, there will be no symptoms of pain, no tenderness to percussion or palpation, and radiographically, the apex will appear completely normal. This is the diagnosis we like to make.
Diagnosis number two is “acute apical periodontitis”. This is an acute diagnosis, so by definition, there will be pain associated with this. And that means pain on percussion and possibly biting as well. Radiographically, the apex should appear normal or at most there might be some thickening of the PDL space. Importantly, you should realize that acute apical periodontitis will often occur along with pulpitis because when inflammation of the pulp occurs, we get an associated inflammation of the periapical tissues. But, the one to watch out for is where we have a normal pulp, and the periapical area is inflamed due to something like occlusal trauma or acute sinusitis. Obviously in this case performing root canal treatment isn’t going to lead to resolution of the symptoms.
The third diagnosis is ‘chronic apical periodontitis’. So the difference here is the word chronic. By definfition this is not a painful condition. This diagnosis is almost always accompanied by a necrotic pulp and the infection in the pulp is causing a periapical lesion which is picked up on a radiograph. In most cases, the pulp test will be negative, but occasionally, if the pulp is only partially necrotic, then you may still get a positive pulp test. The tooth may be slightly tender to percussion as well.
Our fourth diagnosis is ‘acute periapical abscess’. So this is an acute diagnosis so we have pain, the pulp will be necrotic so we’ll usually get a negative pulp test, there should be a lucency obvious radiographically. With a diagnosis of abcess the tooth will be very tender to percussion, often even with a gentle finger tap, and the tooth may be painful to bite on and may even be elevated in it’s socket. There can be localized swelling and lymph node enlargement as well.
Our fifth diagnosis is “chronic apical abscess”. Again because this is a chronic condition, there shouldn’t be symptoms of pain, and the key finding here is that of a sinus tract. The pulp will usually be completely necrotic, so expect a negative pulp test and a radiographic lucency. Because this diagnosis is due to the tooth being associated with an abscess, but the pus that is forming is being released through the sinus tract, these teeth are rarely symptomatic at all. You should be able to place a GP point into the sinus tract and take an x-ray to trace the sinus to a root tip.
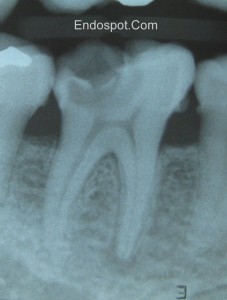
The sixth and final diagnosis I want to talk about today is condensing osteitis. You don’t find a lot of information about this in the literature. It’s a diagnosis that you make radiographically by seeing an increased density of bone around an apex. Usually this will be associated with a pulp that is chronically inflamed but still vital, and the body has responded by increasing the bone density around the apex. I’ll put a reference for a case series in the show notes on the website.
So that’s it for periapical diagnosis. You need to be aware that twhat I’ve described is is a simple clinical diagnosis classification system designed to help you determine what treatment should be provided. There are always exceptions and you might find situations that don’t exactly fit for example when an abscess forms very quickly after pulpal necrosis but the periapical lesion doesn’t expand to a size that produces a lucency on a radiograph. Certainly the diagnoses we discussed tend to require a radiographic component, but it should be the clinical picture and symptoms that your patient is describing which heads you towards your diagnosis. There are also a bunch of conditions that can present as a lucency on an xray which are not endodontic in origin so again, your clinical history and tests should fit the radiographic appearance.
If you want a thorough review of the interaction of the periapical pathologies then go and grab Abbot’s article in Endodontic Topics, reference will be in the show notes. There are also some less common situations where other diagnoses are appropriate such as transient apical periodontitis and if you want to look that up I’ll put the reference for that in the notes too.
And in the meantime, remember you can go to the site and sign up to receive the endospot directly into your email box. That’s it for today. I’ll look forward to speaking to you next time.
Podcast: Play in new window | Download


Hi pat Eli Burger again,
Is condensing osteitis only associated with pulpal disease, or can is result from occlusal trauma to the periapical tissues?
Cheers
Hi Eli,
Generally, Condensing Osteitis is only associated with pulpal disease and should be managed as such.
Pat